Breast Cancer Awareness
Breast cancer still affects 1 in 8 women (13%) in the United States. Breast Cancer Awareness Month began 36 years ago in October 1985 as a collaboration between the American Cancer Society and the pharmaceutical arm of Imperial Chemical Industries (now AstraZeneca) with the goal to provide facts about breast cancer and promote early detection methods. In 1973, former child star and US Ambassador Shirley Temple Black went public with her cancer diagnosis and mastectomy. Betty Ford is widely credited with removing much of the stigma and secrecy surrounding breast cancer. She was diagnosed and underwent mastectomy surgery shortly after moving to the White House in 1974. Following her example, Happy Rockefeller, the Second Lady found a lump and underwent surgery a few weeks after Mrs. Ford.
These early high-profile women paved the way for the current climate of openness, hope and possibilities. However over 43,000 US women will still die from breast cancer this year. 280,000 new cases of invasive breast cancer plus nearly 50,000 new cases of the non-invasive type are projected in 2021. With the exception of skin cancer, death due to breast cancer in women is higher than any other type. It is the most commonly diagnosed cancer around the world according to the World Health Organization. Black women are more likely to die from breast cancer overall.
Health care professionals from front line staff to executives are still debunking the many myths, wives-tales and other misinformation that exist in popular culture today.
Common Myths
- Finding a lump in my breast means I have cancer: only a small number of lumps are actually cancer but it is important to monitor any changes in your breast tissue.
- Mammograms can cause breast cancer to spread: mammograms require a small amount of radiation exposure and along with self-exam, offer the best method of early detection.
- Breast cancer is contagious: That was a new one for me. You cannot catch it or transfer it to anyone else.
- Deodorants/Anti-perspirants can cause breast cancer: no scientific evidence is available to support this claim
- Men cannot get breast cancer: Each year roughly 400 US men die from breast cancer. New cases in men are expected to be around 2500 this year. Breast cancer in men is a small but very real risk and men need to monitor changes in their breast tissue as well.
- No family history so I am safe: Only 5-15% of breast cancers are hereditary in nature meaning 85% occur in women with no family history.
- My healthy lifestyle means I am safe: a proper diet, exercise and overall smart lifestyle choices will mitigate risk but does not eliminate it.
- Wearing a bra (especially underwire) causes breast cancer: This myth is floated out by the media every so often but wearing a bra does not constrict the flow of lymph fluids. A 2014 study of 1500 breast cancer patients found no correlation to support this claim.
- Carrying your cell phone in your bra causes breast cancer: This appears to be another media generated myth started by a noted TV doctor in 2013. The manufacturers of cell phones do recommend keeping them away from your body as much as possible. Cell phones do emit low-level radiation as opposed to the high-energy radiation in X-rays.
- A sweet tooth can cause breast cancer: there is no evidence linking sugar consumption with breast cancer or that it somehow ‘feeds’ the cancer cells. However, being overweight is an established risk factor in cancer.
- No lump therefore no cancer: just because you cannot feel it does not mean it is not there. This is not a valid excuse to avoid mammograms. This is just as incorrect as ‘if it hurts it’s not cancer’ or ‘if it’s smooth and rolls around, it’s not cancer.’
FAQ’s
In addition to these myths and misconceptions medical professionals still frequently field questions like the following:
- Does drinking milk increase my risk? There is limited research and limited evidence to support this versus the benefits of dairy consumption like calcium, potassium, and phosphorus.
- Can hair dye or chemical straighteners cause cancer? A National Institute of Health study in 2019 found evidence that using chemical straighteners every 5-8 weeks increases your risk by 30%.
- Does smoking and/or drinking alcohol cause cancer? Smoking and second-hand smoke are known risk factors. With alcohol, moderation is the key. Having more than one per day has been shown to increase cancer risk.
- Can my birth control pills cause breast cancer? The risk is much smaller today than in my mother’s day due to lower amounts of hormones used in the pills. Your risk does go up with prolonged use. There is some thought that it is best to do the 5 years on/1 year off sequence.
- Am I too young to get breast cancer? In 2017, 27% of women 60-70 were diagnosed, 23% in women in their 50’s. 4% were diagnosed in women under 40. 4% is not ZERO.
- If I am done with treatment, am I done with breast cancer? Recurrence rates are highest from 2-5 years out, so the benchmark has been 5 years. However, cancer is tricky and insidious, so vigilance is necessary. There are other long-term effects of treatment including physical (pain, fatigue, skin/hair changes, neuropathy) as well as mental and emotional effects like anxiety and fear, not to mention the effect on our loved ones. The myth is that you are ‘back to normal’ but your normal has now changed. Everyone is unique as is their cancer and their path through it.
- Does breast feeding prevent breast cancer? The short answer is yes. Read this 2014 article from MD Anderson for further information.
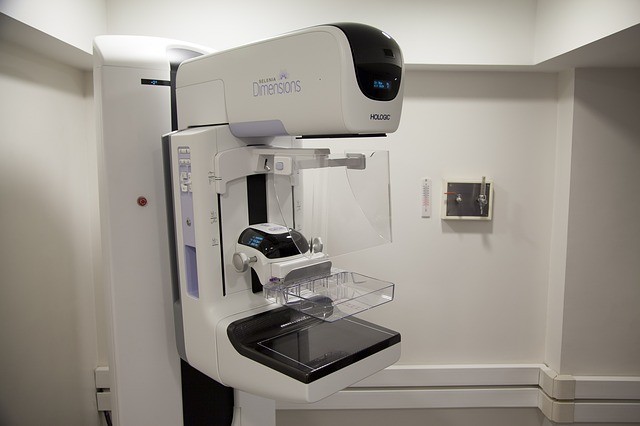
Healthcare faced many challenges this past year. COVID-19 affected access to routine screenings. With screenings down, early detection rates are presumed to be down. Screening facilities have safety precautions in place and breast cancer screening should be considered an ‘as soon as possible’ procedure. Screenings cannot prevent breast cancer, but are key in early detection. Early detection means early intervention; increasing success rates significantly. The good news is that death rates have remained steady for women under 50 but have decreased by about 1% per year in older women. Overall death rates have declined by 40% from 1989-2016 largely due to better awareness, early detection, and better treatments. There are 3.8 million breast cancer survivors in the US today! Healthcare professionals understand the need for more education, screenings, funding, and support. It is vital to women & men (and the people who love them) everywhere that we use whatever power we have to empower each other.
NHS Solutions has experienced interim healthcare leaders available for assignments in the often difficult-to-fill area of oncology. Contact us to discuss your organizations needs. Our services span the entire United States.
